Neuropsychotherapy in continuing professional development: Is it really helpful in mental health professions?
Zhi Xiang On
The University of Melbourne
Pieter Rossouw
Mediros Clinical Solutions and the Neuropsychotherapy Institute

On, Z. X., & Rossouw, P. J. (2015). Neuropsychotherapy in continuing professional development: Is it really helpful in mental health professions?. International Journal of Neuropsychotherapy, 3(2), 131–138. doi: 10.12744/ijnpt.2015.0131-0138
Abstract
Continuing professional development (CPD) is a mandatory requirement in many mental health professions, and it is a common practice in Australia. Despite the emphasis placed on CPD within the field of psychology, there is minimal empirical evidence concerning the impact of CPD on the development of psychologists. CPD training comes in different forms. While neuropsychotherapy is a fairly new paradigm in the field of psychotherapy, currently with around 10,000 clinicians trained in this modality, neurobiological research has shown that it contributes to the enhancement of positive behavior, brain functioning, and brain structure. Understanding the neurobiological effect of talking therapy will in turn create a new tool for psychologists to improve their practice. A multi-pronged research program, undertaken by the authors, is aimed at addressing some of these gaps by looking at the effectiveness of CPD in psychologists’ development with a neuropsychotherapy focus. The present study found that CPD has an impact on the knowledge, skills, and adeptness of psychologists in clinical practice. These studies are expected to shed some light on the implementation of CPD in Australia and the impact of neuropsychotherapy training on psychologists’ clinical practice.
Key words: continuing education, continuing professional development, neuropsychotherapy
To ensure the continuing development of mental health professionals throughout their working lives, it is important that they take part in continuing professional development (CPD). By participating in CPD activities, mental health professionals can advance their knowledge, skills, and understanding of a diversity of treatment approaches (Belar & Perry, 1992; Bloom, 2005). CPD also has an important role among health professions in fostering the incorporation of science into clinical practice and supporting the use of evidence-based practices (Psychology Board of Australia, 2012). In order to keep up to date with scientific developments, constant participation in CPD is essential; it both facilitates a greater understanding of client care processes and health outcomes and enhances practitioners’ ability to adapt to the changing needs of clients (Bloom, 2005; Psychology Board of Australia, 2012). In sum, CPD ensures the long-term development of the core competencies of a psychologist—because psychologists are required to ensure that their therapeutic approaches are in line with the current research evidence.
Participation in CPD is mandatory for psychologists in Australia who wish to renew their registration (Psychology Board of Australia, 2010). The Psychology Board of Australia utilizes a self-directed and self-regulatory CPD model that emphasizes psychologists’ assessment, monitoring, and evaluation of their own developmental needs throughout their careers. Encompassed in this model is the expectation that psychologists assess their existing competence, knowledge, and skills; that they develop, monitor, and reflect upon their individual learning plans; and that they evaluate the objectives of CPD activities and learning outcomes in light of their individual learning objectives (Psychology Board of Australia, 2010, 2011, 2012). Although it is a mandatory requirement, a recent study has shown that only 80% of registered psychologists attend these professional development activities, including seminars, workshops, and conferences, and around 4% of the current registered psychologists reported that they had not taken part in any professional development training in the 12 months prior to the study (Grenyer, Mathews, Stokes, & Crea, 2010). The authors suggested that the reason for this may be that CPD was not a mandatory requirement at the time of the survey. However, no follow-up study has been done with regard to this matter since CPD became a mandatory requirement.
The Psychology Board of Australia (2012) acknowledges a wide variety of activities that constitute CPD, including: attending seminars, conferences, or workshops; conducting presentations; professional reading of peer-reviewed journals; undertaking postgraduate study and research. Informal activities such as discussions with colleagues and case conferences are also recognized by the Board. It is understandable that the wide range of CPD activities ensures that psychologists can choose a suitable form of training for themselves. For instance, it is important to note that, for adults, learning is most effective in a supportive environment where learners feel safe to make mistakes without consequences (Clapper, 2010; Kaufman, 2003). However, Grenyer, Mathews, Stokes, and Crea (2010) have shown that up to 26% of registered psychologists did not engage in private study/journal reading, or any other relevant reading. Unfortunately, it is difficult to track down informal activities or assess their impact. For most psychologists, formal events such as seminars, conferences, and workshops are still the most popular sources of CPD (Grenyer et al., 2010).
Despite the fundamental role of CPD within psychology, to date there has been remarkably little published research in this area. This dearth of empirical research highlights a considerable gap in our current understanding of the extent to which participation in CPD influences clinical practice, as it is assumed to do. It is similarly assumed that it is beneficial to psychologists who attend CPD. A small number of North American researchers have considered the role of CPD in psychology, mostly through satisfaction-type studies. Overall, most psychologists in North America reported mid-high satisfaction with the quality of CPD (Fagan, Ax, Liss, Resnick, & Moody, 2007; Neimeyer, Taylor, & Philip, 2010; Neimeyer, Taylor, & Wear, 2009; Sharkin & Plageman, 2003). While these studies have provided some insights into psychologists’ perceptions of and expectations for CPD, satisfaction ratings provide little information about what motivates the selection of CPD activities or the extent of new learning that occurred through CPD participation.
Additionally, and perhaps more importantly, satisfaction ratings provide little, if any, understanding of the impact of CPD on clinical practice or client outcomes (Neimeyer et al., 2010). To the best of our knowledge, it appears that only four published studies to date have investigated the extent to which participation in CPD facilitates psychologists’ knowledge and skill development. All these studies reported moderate to high levels of learning through CPD activities (Neimeyer et al., 2009; Neimeyer et al., 2010; Rossouw & Hatty, 2013a, 2013b).
Moreover, psychologists who participated in CPD activities also believed that this could improve their clinical practices (Neimeyer et al., 2009; Neimeyer et al., 2010; Sharkin & Plageman, 2003). According to Daniels and Walter (2002), the lack of formal evaluation of CPD has led to the difficulty in determining to what extent competence, knowledge, and skills are being developed through CPD, and to what extent such learning has an impact on a psychologist’s clinical practice.
The idea of CPD, which has only recently become a mandatory requirement for psychologists, is still an innovation in Australia. Mental health professions still struggle to accept the importance of CPD, and many do not understand what to expect from it (Martin, 2014). Promoting the effectiveness of attending CPD might perhaps encourage more psychologists to attend the training. Reports have also shown that financial constraints are one of the reasons psychologists are not constantly involved in CPD (Grenyer et al., 2010).
Every psychologist adopts different therapeutic approaches in their daily practice. Neuropsychotherapy as an independent theoretical approach is no different in this respect from all other theoretical models, and it has increasingly been widely practiced among psychologists. Neuropsychotherapy looks at mental wellbeing from a multidisciplinary perspective that focuses not merely on neuroscience but also on human biology and psychology in order to enhance the clinical practice of talking therapy. Neuropsychotherapy training provides psychologists with a foundational understanding of the neurobiology of mental life. Knowledge obtained from such training may increase the effectiveness of psychology practices across different types of psychotherapies.
This present study aims to validate the effectiveness of CPD on psychologists’ development and practice. Building on that, it also aims to understand the impact of neuropsychotherapy training and whether it is applicable to psychologists without a background in neuroscience. It is hypothesized that (i) CPD will increase the knowledge of psychologists in current contemporary psychotherapy, and (ii) neuropsychotherapy training will be effective to psychologists with or without a background in neuroscience.
Method
Stage 1
Stage 1 data was collected between March 2013 and January 2015. Following participation in a neuropsychotherapy CPD workshop, mental health professionals were invited to complete a one-page paper-based questionnaire. A total of 3501 participants completed the questionnaire. Participants provided self-assessed ratings of their knowledge, ability, comfort, and understanding of the structure of the brain, the role of neurotransmitters, and the neurophysiology of the brain before and after the workshop. Available demographic data for Stage 1 participants is shown in Table 1.
Table 1
Available Demographic Data for Stage 1 Participants
| N | % of sample | ||
| Workshop type | Depression | 849 | 24.3 |
| BrainAnxiety | 1154 | 33.0 | |
| DevelopingBrain | 579 | 16.5 | |
| DepressionSkills | 152 | 4.3 | |
| AnxietySkills | 197 | 5.6 | |
| Relationships | 367 | 10.5 | |
| AgeingBrain | 144 | 4.1 | |
| BrainBasedTherapies | 31 | .9 | |
| AnxiousAdolescent | 28 | .8 | |
| Year | 2010 | 415 | 11.9 |
| 2011 | 802 | 22.9 | |
| 2012 | 1225 | 35.0 | |
| 2013 | 609 | 17.4 | |
| 2014 | 416 | 11.9 | |
| 2015 | 34 | 1.0 | |
| Location | Adelaide | 274 | 7.8 |
| Brisbane | 628 | 17.9 | |
| Canberra | 288 | 8.2 | |
| Melbourne | 929 | 26.5 | |
| Perth | 391 | 11.2 | |
| Sydney | 809 | 23.1 | |
| Hobart | 60 | 1.7 | |
| Launceston | 29 | .8 | |
| Cairns | 31 | .9 | |
| Mackay | 62 | 1.8 | |
Results
The data was analysed using IBM® SPSS® v21 Statistical Package for the Social Sciences (IBM Corp., 2012). The data was checked for normality, and outlying cases were removed. Descriptive statistics are displayed in Tables 2 to 6. While the three after workshop variables were negatively skewed, the data was not transformed as doing so would make interpretation more difficult. The analysis focused on comparisons of self-reported before and after workshop ratings of knowledge, ability, and comfort in using the information. Paired sample t-tests were used to conduct total sample comparisons with effect sizes calculated using Equation 8 outlined by Morris and DeShon (2002).
Table 2
Descriptive Statistics for Before and After Workshop Questions Assessing Knowledge, Ability, and Comfort in Using Information
| % of responses | ||||||||
| n | 1 | 2 | 3 | 4 | 5 | m | SD | |
| Overall knowledge of the topic covered | ||||||||
| before the workshop | 3493 | 13 | 33 | 44 | 9 | 1 | 2.53 | 0.87 |
| after the workshop | 3484 | - | 1 | 16 | 58 | 25 | 4.08 | 0.67 |
| Ability to counsel clients about the topic covered | ||||||||
| before the workshop | 3485 | 17 | 35 | 36 | 11 | 1 | 2.44 | 0.83 |
| after the workshop | 3472 | - | 2 | 22 | 53 | 22 | 3.95 | 0.74 |
| Comfort level in providing services to clients in relation to the topic covered… | ||||||||
| before the workshop | 3465 | 18 | 29 | 33 | 16 | 4 | 2.58 | 1.07 |
| after the workshop | 3467 | - | 3 | 18 | 48 | 30 | 4.05 | 0.79 |
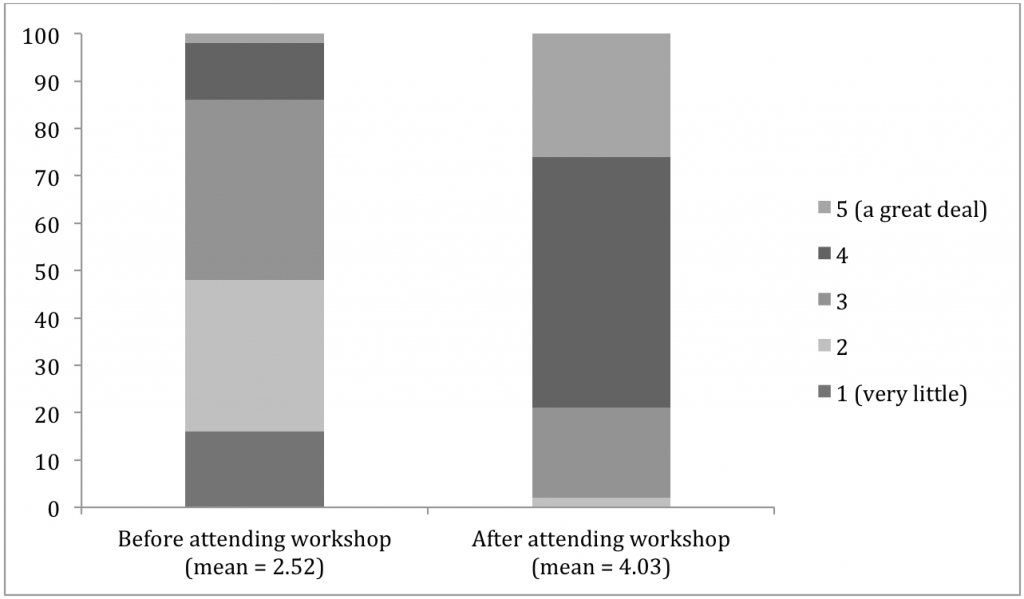
Note. The numbering scale goes from: 1 = very little to 5 = a great deal (see Figure 1).
Total sample analyses suggested statistically significant increases in average ratings of knowledge (t (3483) = −120.99, p < 0.001, 95% CI [−1.58, −1.53], d = −2.00), ability to counsel clients (t (3471) = −113.48, p < 0.001, 95% CI [−1.53, −1.48], d = −1.92), and comfort in providing services (t (3456) = −100.61, p < 0.001, 95% CI [−1.49, −1.44], d = −1.56) after workshop participation compared to before workshop scores.
Figure 1. Results of overall learning before and after the workshop.
Table 3
Descriptive Statistics for Before and After Workshop Questions Assessing Understanding of Structure, Role of Neurotransmitters, and Neurophysiology of the Brain
| % of responses | ||||||||
| n | 1 | 2 | 3 | 4 | 5 | m | SD | |
| The structure of the brain | ||||||||
| before the workshop | 674 | 7 | 30 | 46 | 16 | 2 | 2.76 | 0.85 |
| after the workshop | 676 | - | 2 | 20 | 61 | 17 | 3.94 | 0.66 |
| The role of neurotransmitters in brain functioning | ||||||||
| before the workshop | 675 | 9 | 32 | 43 | 14 | 2 | 2.67 | 0.89 |
| after the workshop | 676 | - | 2 | 21 | 60 | 17 | 3.96 | 1.39 |
| The neurophysiology—or functioning—of the brain | ||||||||
| before the workshop | 673 | 9 | 34 | 43 | 12 | 2 | 2.64 | 0.88 |
| after the workshop | 674 | - | 2 | 21 | 57 | 18 | 3.93 | 0.70 |
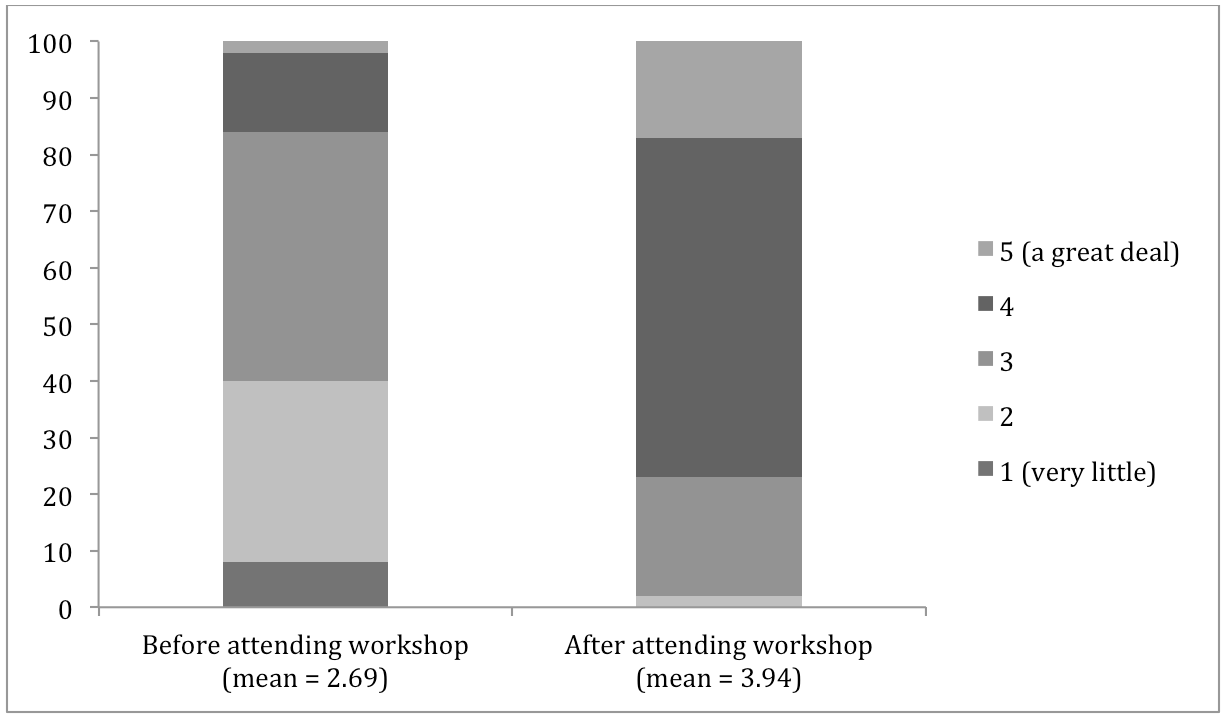
Figure 2. Results of overall neuropsychotherapy knowledge before and after the workshop.
Total sample analyses suggested statistically significant increases in average understanding of the structure of the brain (t (1050) = −56.27, p < 0.001, 95% CI [−1.22, −1.14], d = −1.55), the role of neurotransmitters in brain functioning (t (1049) = −30.21, p < 0.001, 95% CI [−1.37, −1.20], d = −1.11), and the neurophysiology (or functioning) of the brain (t (1048) = −58.43, p < 0.001, 95% CI [−1.33, −1.24], d = −1.62) after workshop participation compared to before workshop scores.
Table 4
Average Differences of Before and After Workshop Questions Assessing Knowledge, Ability, and Comfort in Using Information
| Depression | Brain Anxiety | Developing Brain |
Depression Skills |
Anxiety Skills |
Relationships | Ageing Brain |
Brain Based Therapy |
Anxious Adolescent |
|
| before the workshop | 2.46 | 2.45 | 2.51 | 2.66 | 2.69 | 2.64 | 2.77 | 2.48 | 2.2 |
| after the workshop | 4.04 | 4.07 | 4.01 | 4.04 | 4.05 | 3.93 | 3.96 | 3.74 | 3.67 |
| differences | 1.58 | 1.62 | 1.5 | 1.38 | 1.36 | 1.29 | 1.19 | 1.26 | 1.47 |
The results showed that the brain anxiety workshop had the highest significant differences before and after participants attending the workshop. This is probably due to the fact that this was the first workshop presented in the series and facilitated the biggest impact.
Table 5
Average Differences of Before and After Workshop Questions Assessing Understanding of Structure, Role of Neurotransmitters, and Neurophysiology of the Brain
| Depression | Brain Anxiety | Developing Brain |
Depression Skills |
Anxiety Skills |
Relationships | Ageing Brain |
Brain Based Therapy |
Anxious Adolescent |
|
| before the workshop | 2.68 | 2.43 | 2.59 | N/A | 2.64 | 2.75 | 2.88 | 2.86 | 2.97 |
| after the workshop | 3.93 | 3.85 | 3.98 | N/A | 3.92 | 3.92 | 3.94 | 3.88 | 4.08 |
| differences | 1.25 | 1.42 | 1.39 | N/A | 1.28 | 1.17 | 1.06 | 1.02 | 1.11 |
The results showed that the brain anxiety workshop had the highest significant differences before and after participants attending the workshop, again underlining the effect of introducing the new paradigm in the field.
Table 6
Average Differences of Before and After Workshop Questions Assessing all Questions
| Depression | Brain Anxiety | Developing Brain |
Depression Skills |
Anxiety Skills |
Relationships | Ageing Brain |
Brain Based Therapy |
Anxious Adolescent |
|
| before the workshop | 2.57 | 2.44 | 2.55 | 2.66 | 2.67 | 2.7 | 2.83 | 2.67 | 2.59 |
| after the workshop | 3.98 | 3.96 | 4.00 | 4.04 | 3.98 | 3.92 | 3.95 | 3.81 | 3.88 |
| differences | 1.41 | 1.52 | 1.45 | 1.38 | 1.31 | 1.22 | 1.12 | 1.14 | 1.29 |
The results showed that the brain and anxiety workshop had the highest significant differences before and after participants attending the workshop, underlining the trend described earlier.
The importance of CPD in the professional development of psychologists and other mental health practitioners has been demonstrated by this study. Neuropsychotherapy was found to be user friendly by most of the psychologists who participated. It is also very important to note that most of the CPD workshops included in the present study were neuroscience-based, and future research should look at the effectiveness of CPD with a focus on other psychotherapies in psychologists’ development.
References
Belar, C. D., & Perry, N. W. (1992). National conference on scientist-practitioner education and training for the professional practice of psychology. American Psychologist, 47, 71–75. doi:10.1037/0003-066x.47.1.71
Bloom, B. S. (2005). Effects of continuing medical education on improving physician clinical care and patient health: A review of systematic reviews. International Journal of Technology Assessment in Health Care, 21, 380–385. doi:10.1017/s026646230505049x
Clapper, T. C. (2010). Beyond Knowles: What those conducting simulation need to know about adult learning theory. Clinical Simulation in Nursing, 6, e7–e14. doi:10.1016/j.ecns.2009.07.003
Daniels, A. S., & Walter, D. A. (2002). Current issues in continuing education for contemporary behavioral health practice. Administration and Policy in Mental Health, 29, 359–376. doi: 10.1023/a:1019653123285
Fagan, T. J., Ax, R. K., Liss, M., Resnick, R. J., & Moody, S. (2007). Professional education and training: How satisfied are we? An exploratory study. Training and Education in Professional Psychology, 1, 13–25. doi:10.1037/1931-3918.1.1.13
Grenyer, B. F. S., Mathews, R., Stokes, D., & Crea, K. (2010). The Australian psychology workforce 2: A national profile of psychologists’ education, training, specialist qualifications and continuous professional development. Australian Psychologist, 45, 168–177. doi:10.1080/00050067.2010.482108
Kaufman, D. M. (2003). Applying educational theory in practice. BMJ 326, 213–216. doi:10.1136/bmj.326.7382.213
Martin, J. (2014). The duality of continuing professional development in mental health social work: Voluntary and involuntary status. Australian Social Work, 67, 227–239. doi:10.1080/0312407X.2013.829113
Morris, S. B., & DeShon, R. P. (2002). Combining effect size estimates in meta-analysis with repeated measures and independent-groups designs. Psychological Methods, 7, 105–125.
Neimeyer, G. J., Taylor, J. M., & Philip, D. (2010). Continuing education in psychology: Patterns of participation and perceived outcomes among mandated and nonmandated psychologists. Professional Psychology: Research and Practice, 41, 435–441. doi:10.1037/a0021120
Neimeyer, G. J., Taylor, J. M., & Wear, D. M. (2009). Continuing education in psychology: Outcomes, evaluations, and mandates. Professional Psychology: Research and Practice, 40, 617–624. doi:10.1037/a0016655
Psychology Board of Australia. (2010). Continuing professional development registration standard. Retrieved from
http://www.psychologyboard.gov.au/Standards-and-Guidelines/FAQ.aspx
Psychology Board of Australia. (2011). Guidelines on continuing professional development (CPD). Retrieved from
http://www.psychologyboard.gov.au/Standards-and-Guidelines/FAQ.aspx
Psychology Board of Australia. (2012). Fact sheet and frequently asked questions: Continuing professional development (CPD). Retrieved from http://www.psychologyboard.gov.au/Standards-and-Guidelines/FAQ.aspx
Rossouw, P. J. & Hatty, M. (2013a, March/April). Continuing professional development in psychology: Requirements, assumptions, and the lack of evidence. Neuropsychotherapy in Australia, 20, 8–11.
Rossouw, P. J. & Hatty, M. (2013b). Continuing professional development in mental health professions: Does it really make a difference? In Book of Proceedings. Opening Doors. The 14th International Mental Health Conference 2013 (pp. 126–145). 14th International Mental Health Conference, Surfers Paradise, QLD, Australia, 5–7 August.
Sharkin, B. S., & Plageman, P. M. (2003). What do psychologists think about mandatory continuing education? A survey of Pennsylvania practitioners. Professional Psychology: Research and Practice, 34, 318–323. doi:10.1037/0735-7028.34.3.318
Author Note
Zhi Xiang On, Melbourne School of Psychological Science, University of Melbourne; Pieter Rossouw, Neuropsychotherapy Institute.
Correspondence concerning the article should be addressed to Pieter Rossouw, Mediros Clinical Solutions and the Neuropsychotherapy Institute.
Email: [email protected]